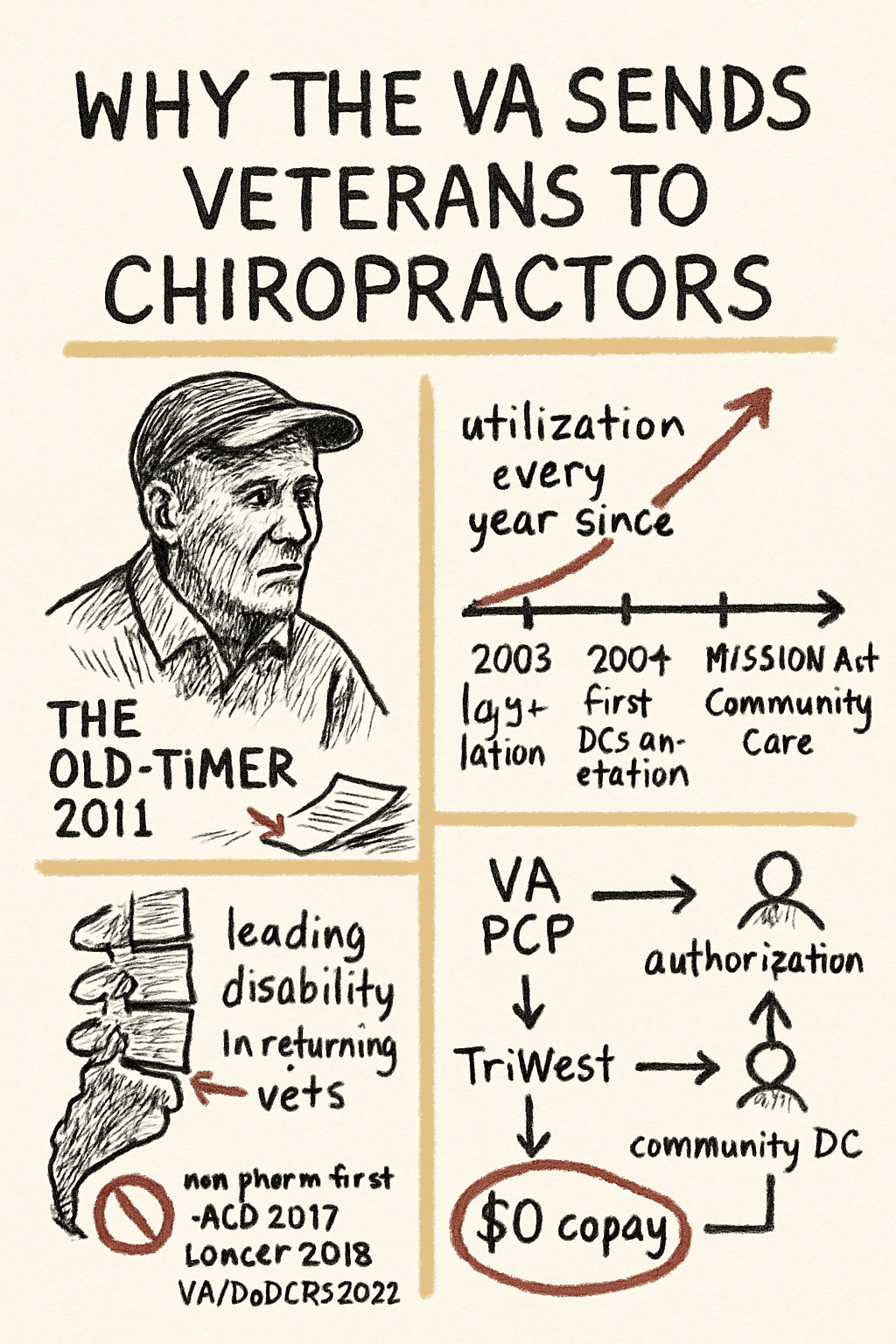
Early in my practice, I had an old-timer come in to claim he was going to be covered by the VA. I thought that wasn’t really likely — you know, government and whatnot. But he showed me an authorization letter from the VA saying they were going to cover the cost of his chiropractic care, so we decided to take a chance.
I’m really glad we did. Over a decade later we’ve treated hundreds of veterans, and it’s been one of the most fulfilling aspects of my career.
I feel like there is a real social contract associated with how we treat the men and women who have served in the Armed Forces. The basic shape of it is this: they risk their lives — or at least agree to be in a situation where they could be called upon to risk their lives — and the rest of us get to enjoy safety, security, and the American dream. I’ve never been asked to risk my life for anything, and I’ve always benefited from their service. So I’m very happy to work with the men and women who have been in the Armed Forces.
That’s the personal version. The bigger story — how the Department of Veterans Affairs ended up sending people like that old-timer to clinics like ours, and where the program is heading next — is also worth telling.
How the VA Got Into Chiropractic
For most of the VA’s history, chiropractic care simply wasn’t on the menu. Veterans who wanted it paid out of pocket or did without.
That changed with the Veterans Health Care, Capital Asset, and Business Improvement Act of 2003 (and earlier related legislation), which directed the VA to provide chiropractic services as part of standard medical benefits. The VA Chiropractic Service was formally established, and on-station chiropractors began appearing in VA medical centers in 2004.
It started small. A handful of facilities. A few dozen chiropractors. The bulk of veterans who needed manual therapy still had to seek it outside the system.
Twenty-some years later, that picture looks completely different. Chiropractic services are now provided in dozens of VA medical centers nationwide, plus a much larger network of community providers (like us) who see veterans through the VA Community Care program. The number of veterans receiving chiropractic care each year has grown substantially — and according to recent forecasting work, it’s projected to keep growing.
What the Forecasting Research Shows
A 2024 paper by Bensel, Corcoran, and Lisi in PLOS ONE — Forecasting the Use of Chiropractic Services Within the Veterans Health Administration — analyzed VA chiropractic utilization data through fiscal year 2022 and projected it forward.
The headline takeaway: utilization has been on a sustained upward trajectory, and the modeling suggests that growth is set to continue. The drivers are familiar to anyone who has watched the VA over the last decade — high prevalence of musculoskeletal conditions among returning service members, an active push to reduce opioid prescribing, growing acceptance of non-pharmacologic care for spine pain, and expanded community-care eligibility under the MISSION Act.
The trend itself isn’t a surprise. Anyone working in veteran care has seen the demand grow firsthand. What the Bensel/Corcoran/Lisi work does is put real numbers on it — and project a future in which chiropractic is an even larger piece of the VA’s MSK and pain-management toolkit than it is today.
Three Reasons the VA Uses Chiropractors
1. Veterans have a lot of musculoskeletal pain
Low back pain is the leading cause of disability among veterans returning from Iraq and Afghanistan. Across the broader veteran population, MSK conditions are consistently among the most-treated complaints. Heavy gear, repeated injuries, the cumulative load of military service — all of it adds up.
If you have a population with that much MSK pain, you need providers who specialize in MSK pain. Chiropractors fit that role naturally.
2. The opioid context
The VA has been working hard for years to reduce opioid prescribing, particularly for chronic pain. That’s a tough problem when the alternative options have to actually work, be acceptable to patients, and scale across a big system.
There’s a growing body of research showing that veterans and other patients who see a chiropractor for spine pain are substantially less likely to be prescribed opioids than otherwise-similar patients who don’t. Whedon and colleagues have published a long line of cohort analyses on this. Lisi’s group has shown the same pattern within the VA system specifically. Manual therapy is one of the credible non-pharmacologic options — not the whole solution, but a meaningful piece of it.
3. The evidence base supports it
National clinical guidelines have steadily moved in the direction of non-pharmacologic care first for low back pain. The American College of Physicians said it explicitly in 2017. The Lancet Low Back Pain Series in 2018 said the same thing globally. Spinal manipulation is a guideline-supported first-line option, alongside exercise, education, heat, and a few other modalities.
The VA’s own clinical practice guidelines — the VA/DoD Clinical Practice Guideline for the Diagnosis and Treatment of Low Back Pain — explicitly include manual therapy in the recommended package of care. When the system’s own guideline tells clinicians to consider it, having providers who specialize in delivering it is a logical move.
How a Veteran Actually Ends Up at a Community-Care Chiropractor
In practice, the path looks roughly like this:
- A veteran with a relevant MSK complaint sees their VA primary care or specialty provider.
- The provider determines that chiropractic care is appropriate, and that on-station VA chiropractic isn’t the right fit (commonly: distance, capacity, scheduling).
- The local VA generates a Community Care authorization through TriWest (the third-party administrator that handles VA Community Care in our region).
- The veteran is matched with — or chooses — a community provider like us. We receive the authorization. Care begins.
- Billing goes through TriWest. The veteran has no copay or out-of-pocket for authorized services in the vast majority of cases.
If a veteran’s case calls for a Nexus letter to support a disability claim — a medical opinion connecting a current condition to military service — that’s something we write when the clinical picture supports it. (More on that on our veterans page.)
The whole process is more bureaucratic than it should be in places, and authorizations get stuck more often than they should. We help patients navigate that part. After more than a decade of doing this, we’ve seen most of the variations.
Why We Take It Seriously — and Where This Is Going
There’s a tendency in healthcare to treat insurance categories as just billing pathways. VA Community Care, in particular, gets treated by some providers as a slow-pay nuisance.
We don’t think about it that way. The veteran in front of us today did something on behalf of the rest of us, and the system that’s paying for their care is the country fulfilling part of its end of that bargain. The least we can do is treat the visit as a real visit — not a paperwork problem.
That’s why our Veterans page leads with the social-contract framing. It’s also why we offer the same evidence-informed care to veterans that we offer everyone else: spinal manipulation, therapeutic massage under the same authorization when clinically indicated, shockwave therapy for stubborn tendinopathies, and rehab. No woo. No tier system. Same standards.
Putting the personal and the systemic together: more veterans are getting chiropractic care every year, the VA is increasingly invested in non-pharmacologic spine and MSK care, and forecasting work suggests that line keeps going up. That’s a good outcome on basically every dimension we care about — for veterans, for the system, for the chiropractic profession’s continued maturation as a serious clinical discipline.
If you’re a veteran with VA Community Care eligibility (or you’re not sure), reach out. We’ve been doing this for over a decade and we know how to help you sort it. If you’re a veteran without Community Care eligibility — or between authorizations — our time-of-service rate and HSA/FSA options are also available.
Either way, thank you for your service. And let’s get to work.
References
- Bensel SH, Corcoran KL, Lisi AJ. Forecasting the Use of Chiropractic Services Within the Veterans Health Administration. PLOS ONE. 2024. PubMed
- Lisi AJ, Brandt CA. Trends in the Use and Characteristics of Chiropractic Services in the Department of Veterans Affairs. Journal of Manipulative and Physiological Therapeutics. 2016;39(5):381–386. PubMed
- Goertz CM, Long CR, Vining RD, et al. Effect of Usual Medical Care Plus Chiropractic Care vs Usual Medical Care Alone on Pain and Disability Among US Service Members With Low Back Pain. JAMA Network Open. 2018;1(1):e180105. PubMed
- Whedon JM, Toler AWJ, Goehl JM, Kazal LA. Association Between Utilization of Chiropractic Services for Treatment of Low Back Pain and Use of Prescription Opioids. Journal of Alternative and Complementary Medicine. 2018;24(6):552–556. PubMed
- Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians. Annals of Internal Medicine. 2017;166(7):514–530. PubMed
- VA/DoD Clinical Practice Guideline. Diagnosis and Treatment of Low Back Pain. 2022. VA/DoD CPG
- Foster NE, Anema JR, Cherkin D, et al. Prevention and Treatment of Low Back Pain: Evidence, Challenges, and Promising Directions. The Lancet. 2018;391(10137):2368–2383. PubMed
This information is provided for educational purposes and should not replace personalized medical advice from a qualified healthcare professional.
Made it to the end. Want the next one in your inbox?
Evidence-informed musculoskeletal content from Dr. Jason Young. One email when something new lands. Unsubscribe anytime.